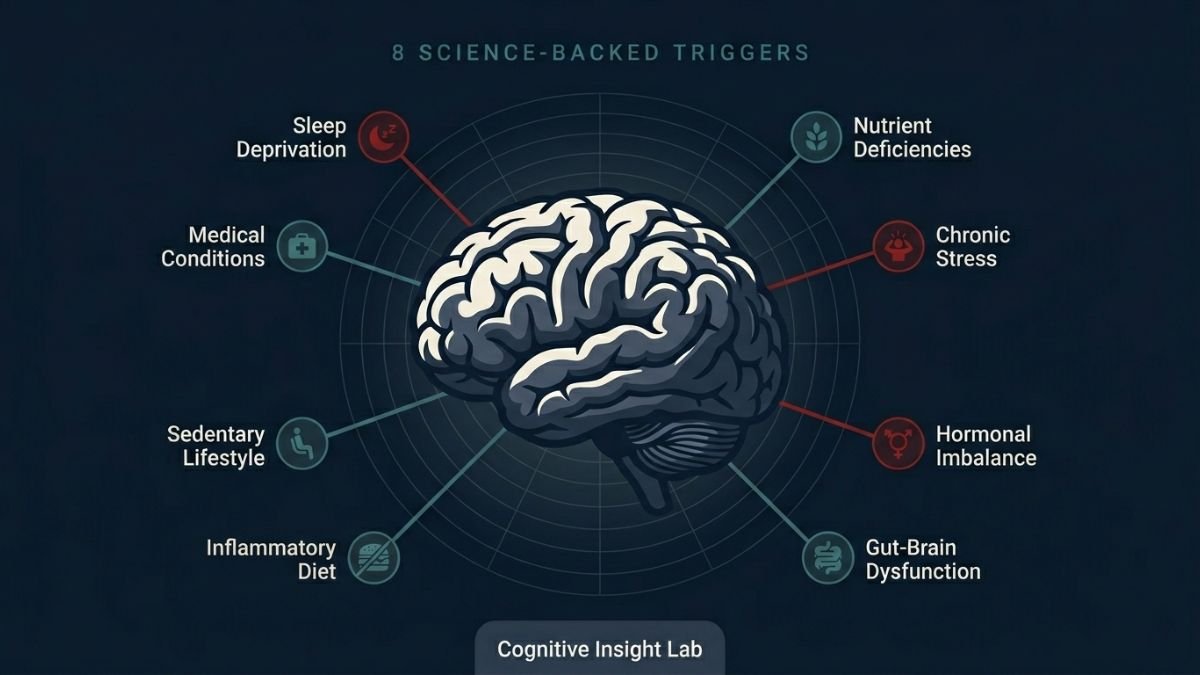
Brain Fog Causes in Adults: 8 Science-Backed Triggers You Need to Know
Medical Disclaimer: This content is for informational and educational purposes only. It does not constitute medical advice and is not intended to diagnose, treat, cure, or prevent any medical condition. Please consult your healthcare provider before making changes to your diet, supplements, or cognitive health routine.
Brain fog causes in adults are more varied — and more common — than most people realize. If you have been losing your train of thought mid-sentence, struggling to concentrate past 2pm, or feeling like your mind is permanently wrapped in cotton wool, you are not imagining it. According to a 2023 survey by the American Psychological Association, nearly 47% of adults between 30 and 55 report experiencing persistent cognitive fatigue or difficulty focusing on a regular basis.
What makes this condition so frustrating is how quietly it builds. It rarely announces itself as a crisis. It creeps in gradually — the word that won’t come, the meeting where nothing sticks, the task you started three times and still haven’t finished. By the time most adults begin taking it seriously, the fog has already been eroding their daily performance for months.
In practice, what we consistently observe is that brain fog is almost never random. It is a signal — a response to something specific happening in the body or environment. And once you understand what your brain is actually responding to, the path forward becomes considerably clearer.
In this article, we break down 8 science-backed triggers of brain fog in adults, explain the biological mechanisms behind each one, and give you a clear-eyed picture of what the research actually shows — no hype, no oversimplification.
1. Chronic Sleep Deprivation: The Most Common Trigger Adults Dismiss

Of all the brain fog causes in adults, chronic sleep deprivation is simultaneously the most common and the most dismissed. Most adults are aware that poor sleep makes them feel tired. Far fewer understand that the damage goes considerably deeper than fatigue.
During sleep, the brain activates what researchers call the glymphatic system — a waste-clearance mechanism that flushes out metabolic byproducts, including beta-amyloid proteins associated with long-term cognitive decline. A 2019 study published in Science found that even a single night of restricted sleep significantly impairs glymphatic clearance, leading to measurable neural waste accumulation.
The cognitive consequences of chronic sleep restriction include:
- Reduced working memory capacity and slower information retrieval
- Impaired decision-making and reduced capacity for complex reasoning
- Increased susceptibility to mental fatigue and distraction
- Difficulty forming and consolidating new memories
- Emotional dysregulation that compounds concentration difficulties
Worth knowing: The National Sleep Foundation recommends 7 to 9 hours per night for adults aged 26 to 64. Consistently sleeping fewer than 6 hours is associated with a 30% increase in cognitive error rates on complex tasks — even when the individual feels subjectively “fine.”
What makes this trigger particularly insidious is a phenomenon called sleep debt normalization. Chronically under-slept individuals adapt to their impaired state and no longer perceive themselves as cognitively compromised — even when objective tests demonstrate significant deficits. A landmark study from the University of Pennsylvania tracked adults sleeping 6 hours per night across 14 consecutive days. By day 10, their cognitive performance was equivalent to someone who had been awake for 24 hours straight. Yet participants continued to report feeling only “slightly sleepy.”
Their subjective assessment had completely decoupled from objective reality.
2. Nutritional Deficiencies: What Your Brain Is Running Low On

The brain accounts for roughly 2% of total body weight but consumes approximately 20% of the body’s entire energy intake. It is extraordinarily sensitive to nutritional status. Several specific deficiencies are directly and consistently linked to brain fog development in adults.
Vitamin B12 B12 is essential for myelin synthesis — the protective sheath around nerve fibers that enables fast, efficient signal transmission between neurons. Deficiency causes progressive demyelination, which translates directly into slower thinking, persistent memory gaps, and mental fatigue. B12 deficiency is particularly prevalent in adults over 40, vegans and vegetarians, and individuals taking proton pump inhibitors (PPIs) or metformin long-term.
Vitamin D Vitamin D receptors are distributed widely throughout the brain, including in the hippocampus — the region responsible for learning and memory consolidation. A 2020 meta-analysis published in Nutrients found that adults with serum vitamin D levels below 20 ng/mL were significantly more likely to report cognitive fatigue and concentration difficulties than those with optimal levels (above 40 ng/mL).
Omega-3 Fatty Acids (DHA) Docosahexaenoic acid (DHA) constitutes approximately 40% of the polyunsaturated fatty acids in the brain. It supports membrane fluidity, neuronal communication efficiency, and neuroinflammation regulation. Chronically low DHA intake has been consistently associated with impaired executive function and increased susceptibility to cognitive fog.
Iron Iron deficiency — even before it progresses to clinical anemia — affects dopamine synthesis and cerebral oxygen delivery. Adults with ferritin levels below 30 µg/L frequently report significant brain fog, sustained fatigue, and difficulty maintaining attention, even when standard hemoglobin levels appear normal.
| Nutrient | Role in Brain Function | Key Deficiency Signs |
|---|---|---|
| Vitamin B12 | Myelin synthesis, nerve signaling | Memory gaps, mental fatigue, tingling |
| Vitamin D | Hippocampal function, mood regulation | Cognitive fog, low mood, fatigue |
| DHA (Omega-3) | Membrane fluidity, neuroinflammation control | Poor focus, slowed processing |
| Iron | Dopamine synthesis, oxygen delivery | Difficulty concentrating, cognitive fatigue |
| Magnesium | Synaptic plasticity, sleep quality | Anxiety, poor sleep, mental tension |
Practical note: Before supplementing, a comprehensive blood panel is worth the investment. Request ferritin (not just hemoglobin), 25-OH vitamin D, B12, and a full metabolic panel. Supplementing without knowing your baseline can mask deficiencies, create imbalances, or produce no effect at all.
LEARN MORE: Cognitive Exhaustion: Why Your Brain Feels Tired Even When You’re Not Doing Much
3. Chronic Stress and Cortisol Overload

Short-term stress is not harmful — it is by design. Acute stress sharpens focus, accelerates processing speed, and mobilizes cognitive resources. The problem is what happens when that system never gets the signal to stand down.
Chronic stress sustains elevated cortisol — the primary stress hormone — for extended periods. While cortisol is essential for acute cognitive performance, chronic elevation produces the precise opposite effect. Research consistently demonstrates that prolonged cortisol exposure:
- Reduces the volume of the prefrontal cortex — the region responsible for planning, decision-making, and complex reasoning
- Impairs hippocampal neurogenesis — the brain’s capacity to generate new neurons and consolidate memories
- Disrupts neurotransmitter balance, particularly serotonin and dopamine, which govern mood, motivation, and mental clarity
- Promotes neuroinflammation by increasing pro-inflammatory cytokine activity throughout the central nervous system
HPA Axis Dysregulation and Cognitive Fatigue
The hypothalamic-pituitary-adrenal (HPA) axis is the body’s central stress response network. Under chronic activation, the HPA axis becomes dysregulated — producing a pattern sometimes called adrenal fatigue in functional medicine literature, though more accurately described as HPA axis dysfunction.
The cognitive signature is recognizable: difficulty concentrating under pressure, impaired short-term memory, mental exhaustion that does not resolve with rest, and persistent cognitive overwhelm even during simple, familiar tasks.
A 2021 study published in Psychoneuroendocrinology found that adults reporting high chronic occupational stress showed a 23% reduction in working memory performance compared to low-stress controls — independent of sleep quality, age, and education level.
👉 Watch the full video breakdown on our YouTube channel
4. Hormonal Imbalances: The Most Frequently Overlooked Driver
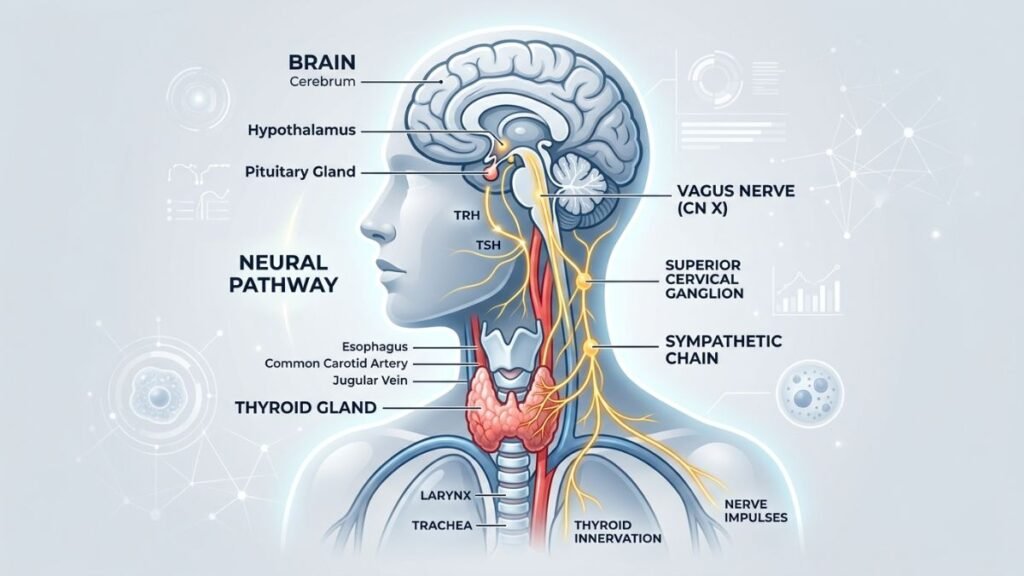
Hormones regulate virtually every aspect of brain function — from neurotransmitter synthesis to cerebral blood flow to synaptic plasticity. When hormone levels fall outside their optimal ranges, the cognitive consequences can be profound and are frequently misattributed to stress, aging, or burnout.
Thyroid dysfunction Both hypothyroidism and subclinical hypothyroidism produce significant cognitive symptoms. The thyroid hormones T3 and T4 directly regulate brain metabolism and neuronal activity. Even subclinical hypothyroidism — where TSH is mildly elevated but T4 remains technically within reference range — is associated with memory impairment, slowed processing speed, and persistent mental fog. This condition affects an estimated 3–8% of the adult population and is frequently missed in standard health screenings.
Perimenopause and menopause The decline in estrogen during perimenopause has direct neurological consequences. Estrogen supports serotonin and acetylcholine activity — both critical neurotransmitters for memory, attention, and mental clarity. Many women in their early-to-mid 40s notice a clear-cut onset of brain fog that correlates with the beginning of perimenopause, often years before conventional menopause markers become clinically apparent.
Testosterone decline in men Testosterone carries neuroprotective properties and supports dopaminergic activity in the brain. Men experiencing andropause — the gradual testosterone decline typically beginning in the late 30s to mid 40s — frequently report reduced mental sharpness, motivational fog, and increasing difficulty with executive tasks and complex decision-making.
Insulin resistance The brain has sometimes been described as the most insulin-sensitive organ in the body. Insulin resistance — increasingly prevalent among adults consuming high-glycemic diets — impairs glucose uptake in brain tissue, directly reducing the energy available for cognitive processing. Researchers at Brown University proposed the term “Type 3 Diabetes” to describe the cognitive deterioration associated with chronic central insulin resistance.
When hormones are the driver: Hormone-related brain fog tends to have a distinct quality — it often appeared at a specific life stage, correlates with other physical symptoms (weight changes, temperature dysregulation, mood shifts, libido changes), and does not respond predictably to sleep or dietary interventions alone. Endocrine evaluation is warranted.
5. Gut-Brain Axis Dysfunction: The Connection Most Adults Miss
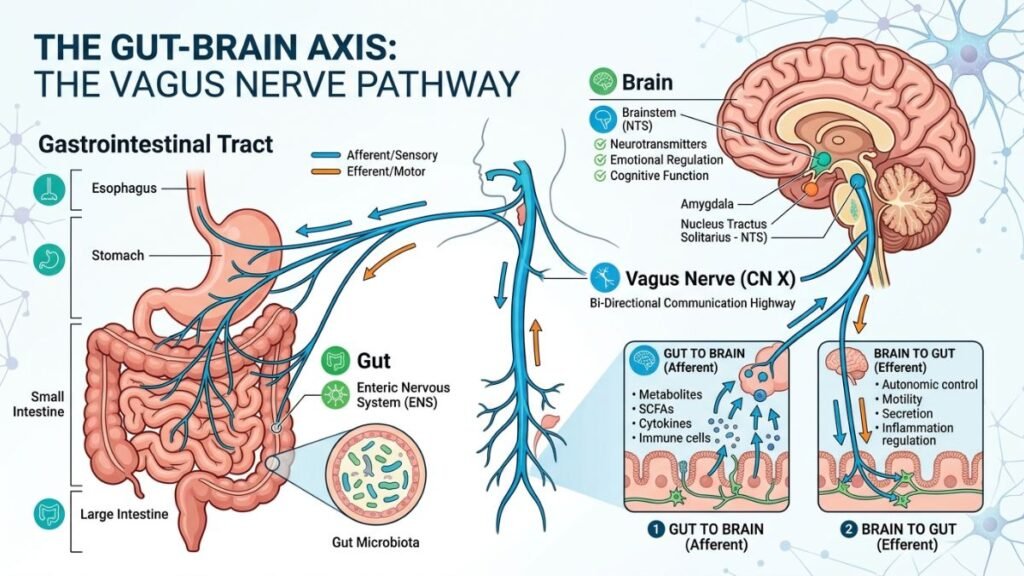
The relationship between gut health and cognitive performance has moved from speculative hypothesis to mainstream neuroscience over the past decade. The gut-brain axis — the bidirectional communication network linking the enteric nervous system with the central nervous system via the vagus nerve — plays a direct and measurable role in cognitive clarity.
The gut microbiome produces approximately 90% of the body’s serotonin and significant quantities of GABA, dopamine precursors, and short-chain fatty acids (SCFAs) that cross into the brain and influence function. Dysbiosis — a significant imbalance in gut microbial composition — has been linked in multiple studies to increased neuroinflammation, impaired blood-brain barrier integrity, and cognitive fog.
The primary gut-related mechanisms driving brain fog include:
- Intestinal permeability (“leaky gut”): When tight junctions in the intestinal wall are compromised, bacterial endotoxins (lipopolysaccharides) enter systemic circulation and trigger brain inflammation
- SIBO (small intestinal bacterial overgrowth): Impairs nutrient absorption — particularly B12, iron, and magnesium — while adding systemic inflammatory load
- Post-antibiotic microbiome depletion: Can reduce SCFA production for months following a course of antibiotics, affecting both mood and cognitive clarity
- High-sugar, low-fiber diets: Selectively deplete beneficial bacterial species while promoting inflammatory populations
A 2022 study published in Nature Mental Health found that individuals with higher microbiome diversity scored significantly better on tests of executive function, working memory, and mental flexibility — independent of age, education, and lifestyle factors.
6. Sedentary Lifestyle and Reduced Cerebral Blood Flow

Physical movement is one of the most powerful — and most consistently neglected — cognitive performance tools available. The underlying mechanism is direct: aerobic exercise increases cerebral blood flow, stimulates the release of brain-derived neurotrophic factor (BDNF), and promotes neurogenesis in the hippocampus.
Conversely, sustained sedentary behavior reduces cerebral perfusion, depresses BDNF levels, and accelerates age-related cognitive decline. A 2020 study in JAMA Network Open found that adults sitting for more than 10 hours per day showed measurable reductions in hippocampal volume compared to more active counterparts — with effects visible in adults as young as 35.
The cognitive impact of chronic inactivity presents as:
- Reduced mental stamina and faster-onset cognitive fatigue
- Slower recall and memory retrieval
- Decreased capacity for sustained, deep attention
- Lowered mood and motivational drive, which compounds cognitive difficulties
The good news is that even modest interventions produce measurable results relatively quickly. A 20-minute brisk walk increases prefrontal cortex oxygenation and improves performance on working memory tasks for up to 2 hours post-exercise — a finding replicated consistently across multiple independent research groups. This does not require a gym membership or a dedicated fitness routine. It requires movement.
A pattern we consistently observe: Adults who introduce a 20-minute walk at lunchtime frequently report that it is the single most effective change they made for afternoon cognitive clarity — more impactful than caffeine, supplements, or dietary adjustments made simultaneously.
7. Inflammatory Diet and Chronic Neuroinflammation
The standard Western diet — high in refined carbohydrates, industrial seed oils, artificial additives, and ultra-processed products — is increasingly recognized by neuroscientists as a significant driver of chronic low-grade neuroinflammation. This type of inflammation does not produce acute symptoms. It does not cause pain or fever. Instead, it manifests as a gradual, cumulative dulling of cognitive clarity — a fog that builds over months and years, often without a clear moment of onset.
Specific dietary contributors to brain fog in adults include:
Refined sugar and high-glycemic foods These produce rapid blood glucose spikes followed by sharp drops, creating cycles of cognitive crash and recovery throughout the day. The afternoon slump that millions of adults experience between 2pm and 4pm is, in many cases, a direct consequence of a high-glycemic lunch.
Industrial seed oils and excess omega-6 fats Soybean, corn, sunflower, and safflower oils are found in nearly every processed food product. At the ratios found in modern diets, excess omega-6 fatty acids promote the production of pro-inflammatory prostaglandins that can cross the blood-brain barrier and exacerbate neuroinflammation.
Alcohol Even moderate regular consumption — two to three drinks per day — impairs sleep architecture (particularly slow-wave and REM sleep), depletes B vitamins, and increases neuroinflammatory markers. Adults who eliminate or substantially reduce alcohol frequently report significant improvements in cognitive clarity within 2 to 4 weeks.
Environmental toxic load Chronic low-level exposure to mold (mycotoxins from water-damaged buildings), heavy metals (mercury, lead), and certain pesticide residues has been linked to persistent cognitive impairment in susceptible individuals. Mycotoxin exposure is a particularly underrecognized driver of treatment-resistant brain fog in functional and integrative medicine settings.
8. Underlying Medical Conditions That Present as Brain Fog
Sometimes, persistent brain fog is not primarily a lifestyle issue. It is a symptom — and it is pointing toward an underlying medical condition that requires direct professional evaluation. Several conditions are particularly and consistently associated with cognitive fog in adults.
Autoimmune conditions Lupus, multiple sclerosis, rheumatoid arthritis, and Hashimoto’s thyroiditis can all produce significant cognitive fog through inflammatory and autoimmune mechanisms that affect the central nervous system. “Lupus fog” and “MS fog” are formally recognized clinical phenomena with documented neurological substrates.
Long COVID cognitive syndrome Post-COVID cognitive impairment affects an estimated 10–30% of individuals who experienced COVID-19, with symptoms persisting for months or years after acute recovery. Proposed mechanisms include microclotting in cerebral vasculature, sustained neuroinflammation, mitochondrial dysfunction, and persistent immune activation affecting brain tissue.
Fibromyalgia “Fibro fog” is one of the most consistently reported symptoms of fibromyalgia — characterized by confusion, significant memory difficulties, and impaired word retrieval. It frequently precedes or accompanies the physical pain symptoms.
Undiagnosed adult ADHD Adult ADHD presents as chronic mental disorganization, difficulty sustaining focus on non-stimulating tasks, and a persistent sense of cognitive inefficiency — symptoms that are easily and commonly misattributed to stress, burnout, or lifestyle-related brain fog. Research estimates that up to 75% of adults with ADHD remain undiagnosed.
When to seek medical evaluation: Brain fog that persists longer than 4 to 6 weeks, worsens progressively over time, is accompanied by other physical or psychological symptoms, or does not respond to lifestyle improvements warrants a comprehensive medical assessment. At minimum, this should include thyroid function tests (TSH, free T3, free T4), complete blood count, metabolic panel, ferritin, 25-OH vitamin D, and B12.
Why Most Adults Have More Than One Trigger
One of the most consistent clinical observations about brain fog causes in adults is that they rarely operate in isolation. Sleep deprivation amplifies cortisol dysregulation. Chronic stress impairs gut barrier integrity. Nutritional deficiencies reduce sleep quality. A sedentary lifestyle worsens insulin sensitivity and depresses BDNF.
This interconnection explains why single-factor interventions frequently produce only partial results. Addressing brain fog effectively tends to require a systematic approach — identifying the primary driver while simultaneously supporting the foundational pillars of cognitive health: sleep, nutrition, stress regulation, physical movement, and gut integrity.
Important Notice: This article is for informational and educational purposes only. The information provided does not constitute medical advice and is not a substitute for professional medical evaluation, diagnosis, or treatment. Brain fog can be a symptom of various underlying health conditions, some of which require medical attention. If you are experiencing persistent cognitive difficulties, please consult a qualified healthcare provider for appropriate assessment and guidance.
Conclusion
Brain fog in adults is not a character flaw, a sign of aging, or something you simply have to accept as the cost of a busy life. It is a signal — and signals, by definition, are telling you something specific.
The eight triggers covered here — sleep deprivation, nutritional deficiencies, chronic stress, hormonal imbalances, gut-brain axis dysfunction, sedentary behavior, inflammatory diet, and underlying medical conditions — account for the substantial majority of adult brain fog cases. What makes this actionable is that most of these triggers respond meaningfully to targeted intervention once they are correctly identified.
Three things worth carrying forward from this article:
- Identify before you intervene. Understanding your specific triggers through testing and careful observation is more effective than adopting generic “brain health” habits without direction.
- Address the foundations first. Sleep, nutrition, movement, and stress regulation are not optional extras — they are the core infrastructure on which everything else depends.
- Take persistence seriously. Brain fog that does not meaningfully improve after 4 to 6 weeks of lifestyle changes deserves professional evaluation, not more patience.
Your cognitive clarity is not fixed. It is dynamic — and the biology that underlies it can be influenced at any age. Save this article for reference, apply what is relevant to your situation, and consider sharing it with someone who might recognize their own experience in these pages.
Frequently Asked Questions
Is brain fog an actual medical condition?
Brain fog is not a formal clinical diagnosis but rather a descriptive term for a cluster of symptoms — including mental fatigue, difficulty concentrating, impaired memory, and slowed thinking. It can be a symptom of various underlying conditions or lifestyle factors. A healthcare provider can help identify the specific root cause through appropriate history, examination, and testing. Never attempt to self-diagnose the cause of persistent cognitive symptoms.
How long does brain fog typically last in adults?
Duration depends almost entirely on the underlying cause and how promptly it is addressed. Fog triggered by acute sleep deprivation or dietary imbalance can begin improving within days once the cause is corrected. Fog associated with nutritional deficiencies or hormonal imbalances may persist for weeks or months until the root issue is appropriately treated. Persistent brain fog lasting beyond 4 to 6 weeks — particularly if worsening — warrants professional evaluation.
Can brain fog be a warning sign of something serious?
In most adults, brain fog reflects correctable lifestyle or nutritional factors. However, it can also be an early presenting symptom of conditions such as thyroid dysfunction, autoimmune disease, Long COVID syndrome, or undiagnosed adult ADHD. If brain fog is worsening, accompanied by other physical or psychological symptoms, or failing to respond to lifestyle modification, a healthcare provider assessment is appropriate and important.
What is the most effective way to start clearing brain fog?
There is no universal rapid fix, but the interventions most consistently associated with improvement are: prioritizing 7 to 9 hours of quality sleep, identifying and correcting nutritional deficiencies through targeted blood testing, substantially reducing refined sugar and ultra-processed food intake, and incorporating daily aerobic movement of at least 20 to 30 minutes. Most adults who address their primary trigger notice meaningful improvement within 1 to 3 weeks.
Does brain fog inevitably get worse as you age?
No. Cognitive fog is not an inevitable feature of aging. While certain age-related shifts — hormonal changes, reduced sleep quality, increased baseline inflammation — can make adults more susceptible to brain fog as they enter their 40s and 50s, the triggers discussed in this article are addressable at any age. Cognitive resilience can be actively maintained and genuinely improved well into later adulthood.
Can chronic stress alone cause persistent brain fog without other contributing factors?
Yes. Sustained psychological stress — particularly when maintained over months or years without adequate recovery — produces measurable structural and functional changes in the brain through cortisol dysregulation, HPA axis dysfunction, and neuroinflammatory mechanisms. Many adults experiencing burnout or chronic work stress report cognitive impairment as their most prominent complaint, often appearing before physical symptoms become apparent.
Is the link between gut health and brain fog well-established scientifically?
The gut-brain axis is now a well-established area of neuroscience research, not a fringe concept. Multiple peer-reviewed studies have documented associations between gut microbiome composition, intestinal permeability, and cognitive function. While the field continues to evolve and causal mechanisms are still being characterized in detail, the clinical evidence for addressing gut health as part of a brain fog intervention strategy is substantial and growing.
Daniel Mercer is a health science writer specializing in cognitive performance, nootropics, and brain health research. With a background in biomedical sciences and over a decade reviewing clinical literature on mental performance and supplementation, he founded Cognitive Insight Lab to cut through the noise and deliver evidence-based analysis for people who take their cognitive health seriously. Daniel does not accept sponsored content and has no financial ties to the brands reviewed on this site.