How to Reduce Brain Fog Naturally: 9 Evidence-Based Strategies That Work
Important Notice: This article is for informational and educational purposes only. The information provided does not replace guidance from a qualified healthcare professional. For personal decisions related to your health, consult a licensed professional.
If you want to know how to reduce brain fog naturally, you are already asking the right question — because the answer is not a single pill or a morning ritual. It is a pattern of interconnected choices that either support or undermine your brain’s ability to function at its best.
Brain fog is one of the most commonly reported cognitive complaints among adults in the United States. A 2022 survey published in the Journal of General Internal Medicine found that over 20% of adults report persistent difficulty with concentration, mental clarity, and memory — numbers that have risen significantly since 2020. Yet despite how common it is, brain fog is not a medical diagnosis. It is a symptom cluster: the mental haze, the word-retrieval failures, the feeling of thinking through wet concrete that tells you something in your brain’s operating environment is off.
What makes brain fog frustrating is that its causes are varied and often overlapping. Poor sleep, chronic stress, inflammatory diet, sedentary behavior, gut dysbiosis, nutritional deficiencies, and hormonal shifts can all contribute — sometimes simultaneously. Understanding which factors are driving your specific experience is the first step toward addressing it with any meaningful precision.
This article covers nine evidence-based strategies for reducing brain fog naturally. Each one is grounded in published neuroscience research and practical enough to implement without overhauling your entire life. You will leave with a clear framework for identifying your most likely contributors and a set of specific, actionable interventions.
What Brain Fog Actually Is — and Why It Happens
Before addressing solutions, it helps to understand the mechanism. Brain fog is not a vague feeling — it has identifiable neurological underpinnings that explain why the interventions below work.
The Role of Neuroinflammation
One of the most well-documented contributors to cognitive sluggishness is neuroinflammation — a state of low-grade immune activation in the brain. When the brain’s immune cells (microglia) become chronically activated — by poor diet, stress, sleep deprivation, or systemic inflammation — they release cytokines that interfere with synaptic transmission and reduce the production of key neurotransmitters including dopamine, serotonin, and acetylcholine.
Research from the NIH has consistently linked elevated inflammatory markers (particularly IL-6 and TNF-alpha) with reduced cognitive performance across multiple domains.
The Prefrontal Cortex Under Load
The prefrontal cortex — the brain region responsible for working memory, decision-making, and executive function — is disproportionately sensitive to stress hormones. When cortisol remains chronically elevated, as it does under sustained psychological stress, prefrontal function deteriorates measurably. This is why people under chronic stress report exactly the symptoms associated with brain fog: difficulty concentrating, poor impulse control, and reduced ability to think clearly.
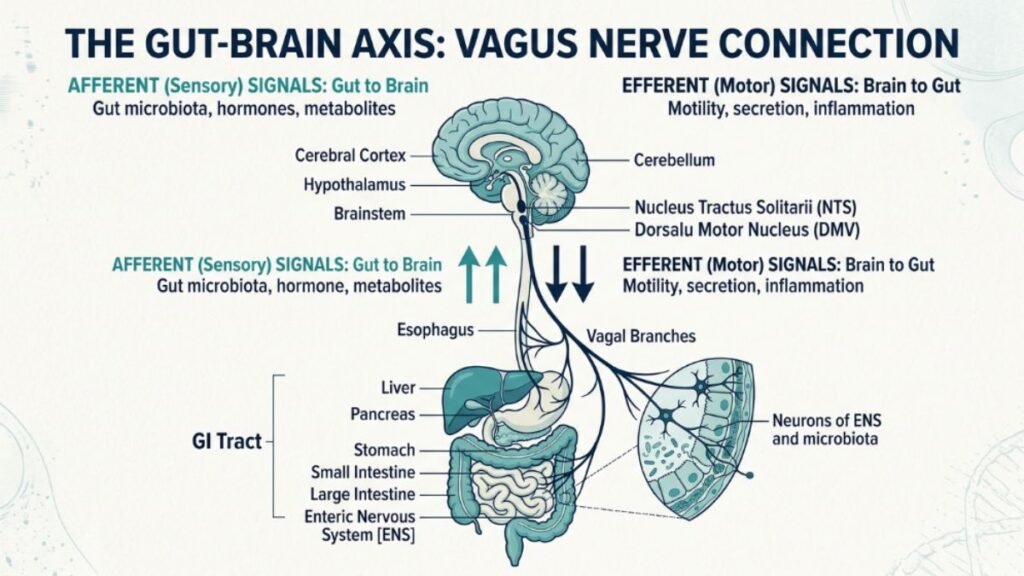
The Gut-Brain Axis
Emerging research has established a bidirectional communication network between the gastrointestinal tract and the central nervous system — the gut-brain axis. The gut microbiome influences brain function through multiple pathways including the vagus nerve, immune system signaling, and the production of neuroactive compounds. Dysbiosis (an imbalance in gut bacteria) has been associated with increased neuroinflammation and reduced cognitive function in multiple published studies.
Practical Tip: Brain fog often has multiple contributing causes operating simultaneously. Addressing only one — say, sleep — while ignoring inflammation or gut health may produce limited results. A multi-system approach consistently outperforms single-variable interventions in the research literature.
1. Prioritize Sleep Architecture, Not Just Sleep Duration
Most adults know they need more sleep. Fewer understand that the quality and structure of sleep matters as much as its duration — and that poor sleep architecture is one of the fastest routes to sustained brain fog.
Why Sleep Stage Distribution Matters
During slow-wave (deep) sleep, the brain’s glymphatic system activates — a waste-clearance mechanism that flushes metabolic byproducts, including amyloid-beta and tau proteins associated with neurodegenerative conditions, from the interstitial spaces between neurons. Research published in Science demonstrated that this clearance system is significantly more active during deep sleep than during wakefulness or light sleep stages.
Disrupted sleep — whether from late-night screens, alcohol, inconsistent sleep schedules, or stress — compresses deep sleep stages and impairs this clearance process. The result is a measurable increase in cognitive sluggishness the following day.
Practical Interventions
- Consistent sleep and wake times — the single most evidence-supported intervention for improving sleep quality. The circadian rhythm is anchored by light-dark cycles and reinforced by behavioral consistency.
- Temperature — core body temperature drops during sleep onset. A room temperature between 65°F and 68°F (18–20°C) facilitates this drop and improves deep sleep proportion.
- Light exposure in the morning — bright natural light within 30–60 minutes of waking anchors the circadian rhythm and improves sleep onset quality the following night.
- Eliminate screens at least 60 minutes before bed — blue light wavelengths suppress melatonin production and delay sleep onset by an average of 90 minutes in controlled studies.
Attention: If you are sleeping 7–9 hours consistently but still waking unrefreshed, consider evaluation for sleep apnea — a common and underdiagnosed condition that severely fragments sleep architecture without the person being aware of it.
2. Address Inflammation Through Diet
The standard American diet — high in refined carbohydrates, industrial seed oils, and ultra-processed foods — is one of the most consistently documented drivers of systemic and neuroinflammation. Shifting the dietary pattern is not about restriction. It is about providing the brain with the raw materials it needs to function and removing the inputs that chronically impair it.
Foods That Drive Brain Fog
| Category | Common Sources | Mechanism |
|---|---|---|
| Refined sugars | Sweetened drinks, baked goods, cereals | Glucose spikes → insulin resistance → reduced brain energy availability |
| Industrial seed oils | Fried foods, packaged snacks | High omega-6 content → pro-inflammatory eicosanoids |
| Ultra-processed foods | Fast food, chips, ready meals | Additives, emulsifiers → gut dysbiosis → neuroinflammation |
| Alcohol | Beer, wine, spirits | Disrupts sleep architecture, depletes B vitamins, increases neuroinflammation |
Foods That Support Cognitive Clarity
- Fatty fish (salmon, sardines, mackerel): Rich in DHA, an omega-3 fatty acid that constitutes approximately 40% of the brain’s polyunsaturated fat content. DHA supports membrane fluidity, synaptic transmission, and anti-inflammatory signaling.
- Leafy greens (spinach, kale, arugula): High in folate, vitamin K, and lutein — micronutrients consistently associated with slower cognitive decline in longitudinal studies.
- Berries: Blueberries in particular contain anthocyanins that cross the blood-brain barrier and reduce oxidative stress in hippocampal neurons.
- Eggs: One of the richest dietary sources of choline, the precursor to acetylcholine — the neurotransmitter most directly involved in memory formation and sustained attention.
- Fermented foods (kefir, kimchi, sauerkraut): Support gut microbiome diversity, which in turn supports the gut-brain axis and reduces neuroinflammatory signaling.
Best Practice: A Mediterranean-style eating pattern — rich in olive oil, fish, vegetables, legumes, and whole grains — has the strongest evidence base of any dietary approach for cognitive protection. A 2022 meta-analysis in Nutritional Neuroscience found consistent associations between Mediterranean diet adherence and reduced cognitive decline across multiple age groups.

3. Regulate Cortisol Through Deliberate Stress Management
Chronic psychological stress is not just uncomfortable — it is neurologically damaging in measurable ways. Sustained cortisol elevation reduces gray matter density in the prefrontal cortex, impairs hippocampal neurogenesis, and disrupts the neurotransmitter balance that underlies clear thinking.
The goal is not to eliminate stress — that is neither possible nor desirable. The goal is to prevent stress from becoming chronic by building reliable physiological downregulation into the daily rhythm.
Evidence-Supported Approaches
Diaphragmatic breathing (physiological sigh): A double inhale through the nose followed by a long exhale through the mouth activates the parasympathetic nervous system within seconds. Research from Stanford University demonstrated that just five minutes of cyclic breathing per day produced measurable reductions in physiological stress markers and self-reported anxiety.
Progressive muscle relaxation: Systematic tensing and releasing of muscle groups reduces both somatic tension and cognitive activation. Studies show effects on cortisol levels comparable to low-intensity aerobic exercise.
Time in nature: A 2019 study in Frontiers in Psychology found that 20–30 minutes in a natural environment significantly reduced salivary cortisol concentrations — with no requirement for active engagement, meditation, or intentional practice.
KNOW MORE: Binaural beats for stress and mental clarity
4. Exercise: The Most Underutilized Cognitive Enhancer
Aerobic exercise is the most robustly supported non-pharmacological intervention for cognitive performance in the scientific literature. It is not a wellness platitude — it is basic neurobiology.
How Exercise Clears Brain Fog
Physical activity elevates the production of Brain-Derived Neurotrophic Factor (BDNF) — a protein that supports the growth, maintenance, and survival of neurons and plays a central role in hippocampal neurogenesis (the formation of new brain cells). BDNF is sometimes described as “Miracle-Gro for the brain” in neuroscience literature, and the analogy is apt.
A single bout of moderate aerobic exercise produces an acute increase in cerebral blood flow that improves attention and working memory within 30 minutes. A 2020 meta-analysis in British Journal of Sports Medicine found that 20–30 minutes of moderate aerobic exercise three to five times per week was associated with significantly improved executive function across all adult age groups studied.
What Kind and How Much
| Exercise Type | Cognitive Benefit | Minimum Effective Dose |
|---|---|---|
| Aerobic (walking, cycling, swimming) | BDNF, cerebral blood flow, executive function | 20–30 min, 3–5x/week |
| Resistance training | Attention, processing speed, memory | 2–3x/week, moderate intensity |
| High-intensity intervals (HIIT) | Acute focus boost, BDNF spike | 10–20 min, 2–3x/week |
| Yoga / tai chi | Cortisol reduction, prefrontal activation | 2–3x/week |
Practical Tip: A 20-minute brisk walk is sufficient to produce measurable cognitive benefits. The threshold for meaningful brain fog reduction through exercise is lower than most people assume. Consistency matters far more than intensity.
👉Check out our content on YouTube

5. Optimize Key Nutritional Deficiencies
Several micronutrient deficiencies are directly linked to cognitive impairment and are common enough in the US adult population to warrant attention before exploring more complex interventions.
The Most Clinically Relevant Deficiencies
Vitamin D: Approximately 42% of American adults are deficient in vitamin D according to data from the National Health and Nutrition Examination Survey (NHANES). Vitamin D receptors are present throughout the brain, and deficiency is consistently associated with increased cognitive complaints, fatigue, and mood disturbances.
Magnesium: Involved in over 300 enzymatic reactions in the body, including multiple processes critical to neurotransmitter synthesis and neuronal energy metabolism. Magnesium glycinate and magnesium threonate are the forms best supported for cognitive and sleep applications.
B vitamins (B6, B9, B12): Essential for the methylation cycle, which produces neurotransmitters and regulates homocysteine levels. Elevated homocysteine is a well-documented independent risk factor for cognitive decline. B12 deficiency is particularly common in adults over 50 due to reduced gastric acid production.
Omega-3 fatty acids (DHA/EPA): As noted above, DHA is a structural component of neuronal membranes. Low plasma DHA is associated with reduced cognitive performance and increased inflammatory signaling.
Attention: Before supplementing, get baseline blood levels tested for vitamin D and B12 in particular. Both deficiency and excess vitamin D carry health risks, and supplementation is most effective when dosing is calibrated to actual blood levels.
6. Support the Gut-Brain Axis
Given the established role of the gut microbiome in modulating neuroinflammation and neurotransmitter availability, gut health deserves direct attention in any comprehensive brain fog strategy.
Practical Interventions for Gut Health
- Increase dietary fiber — fermentable fiber (from vegetables, legumes, and whole grains) feeds the beneficial bacteria that produce short-chain fatty acids with anti-inflammatory and neuroprotective properties
- Add fermented foods — regular consumption of yogurt, kefir, kimchi, or sauerkraut increases gut microbiome diversity; a 2021 Stanford study showed measurable immune and inflammatory benefits from 10 weeks of fermented food consumption
- Reduce ultra-processed food intake — emulsifiers and additives in processed foods disrupt the gut mucosal barrier, contributing to intestinal permeability and systemic inflammation
- Consider a quality probiotic — strains with evidence for gut-brain axis effects include Lactobacillus rhamnosus and Bifidobacterium longum; effects on anxiety and cognitive clarity have been documented in multiple RCTs
7. Manage Hydration and Caffeine
Two of the simplest and most overlooked contributors to brain fog are chronic mild dehydration and caffeine mismanagement.
Dehydration and Cognitive Performance
The brain is approximately 73% water. A fluid deficit of just 1–2% of body weight — well below the threshold of perceivable thirst — produces measurable declines in attention, short-term memory, and psychomotor speed. This is particularly relevant in air-conditioned office environments, where fluid losses are low but cumulative throughout the workday.
Caffeine: Timing Matters More Than Amount
Caffeine’s cognitive benefits are real and well-documented. But timing profoundly affects whether it helps or harms cognitive performance.
Consuming caffeine within the first 60–90 minutes after waking — before cortisol levels have naturally peaked — blunts cortisol’s alerting effect and increases adenosine receptor sensitivity, contributing to afternoon energy crashes. Delaying the first caffeine intake until 90–120 minutes after waking maintains the natural cortisol-driven alertness window and reduces the dependence cycle that contributes to chronic fatigue and brain fog.
Best Practice: Aim for 2–3 liters of water per day (more in hot climates or with physical activity). Delay first caffeine intake until 90 minutes after waking. Avoid caffeine after 2pm to protect sleep architecture.

8. Reduce Cognitive Load Intentionally
Modern knowledge work places extraordinary demands on the prefrontal cortex — the brain region with the highest metabolic cost and lowest recovery capacity. Brain fog is often not a deficiency of anything. It is the result of sustained cognitive output without sufficient recovery.
Structured Rest and Attention Management
Research on ultradian rhythms — 90-minute cycles of high and low neurological alertness that run throughout the waking day — suggests that working with these cycles rather than against them produces better sustained cognitive output.
Practical applications:
- Work in focused blocks of 60–90 minutes followed by 10–20 minutes of genuine rest (not screen switching)
- Single-task rather than multitask — task-switching carries a significant cognitive overhead that depletes prefrontal resources faster than sustained single-task work
- Use deliberate transitions between cognitively demanding activities — a 5-minute walk, a brief breathing practice, or an audio-based relaxation session can meaningfully reset attentional capacity
SEE ALSO: Audio-based cognitive reset program
9. Consider Evidence-Supported Nootropic Supplements
Once lifestyle foundations are in place — sleep, diet, exercise, stress management — targeted supplementation can provide meaningful additional support for cognitive clarity.
The most evidence-supported supplements specifically relevant to brain fog include:
Lion’s Mane Mushroom (Hericium erinaceus): Contains compounds that stimulate Nerve Growth Factor (NGF) synthesis, supporting neuronal maintenance and regeneration. A 2023 study in Scientific Reports found improvements in cognitive performance in healthy adults after 28 days of supplementation.
Bacopa Monnieri: An adaptogenic herb with consistent evidence for improving memory consolidation and reducing cognitive anxiety. Effects typically require 8–12 weeks of supplementation to reach full expression.
Alpha-GPC: One of the most bioavailable choline precursors — choline is the direct precursor to acetylcholine, the neurotransmitter central to memory and focused attention. Well-studied and widely used in clinical cognitive health research.
Rhodiola Rosea: An adaptogen with strong evidence for reducing mental fatigue and cognitive performance decrements under stress, particularly for knowledge workers and students during high-demand periods.
Attention: Supplements interact with medications and individual health conditions. Always consult a healthcare provider before adding nootropic supplements to your routine, particularly if you are taking antidepressants, blood pressure medications, or anticoagulants.
LEARN MORE: Best Supplements for Brain Fog in 2026: Ranked, Reviewed and Compared

Conclusion
Brain fog is not inevitable, and it is not a permanent condition. In most adults, it is a signal from a system under strain — and one that responds well to targeted, consistent intervention.
The nine strategies covered here are not independent — they compound. Improving sleep quality reduces inflammation. Reducing inflammation improves gut health. Better gut health supports neurotransmitter balance. Neurotransmitter balance improves stress resilience. Each intervention you implement makes the next one more effective.
The most important step is to identify your primary driver — whether that is sleep quality, diet, chronic stress, or nutritional deficiency — and address that first before adding complexity. Most people with persistent brain fog will see meaningful improvement within two to four weeks of addressing even one high-impact variable consistently.
Start with one change. Hold it for two weeks. Add another. That is what sustainable cognitive recovery looks like.
Frequently Asked Questions about How to Reduce Brain Fog Naturally
How long does it take to reduce brain fog naturally?
This depends on the underlying cause. If brain fog is primarily driven by sleep deprivation or dehydration, improvements can appear within days of addressing those factors. Diet-related brain fog typically improves within two to four weeks of dietary change. Supplementation-based approaches (bacopa, lion’s mane) generally require eight to twelve weeks to produce measurable effects. Addressing neuroinflammation through combined lifestyle changes produces the most sustained results and typically shows meaningful improvement within four to six weeks.
Can brain fog be a sign of something serious?
Yes, in some cases. Persistent brain fog that does not respond to lifestyle interventions — particularly when accompanied by severe memory loss, personality changes, extreme fatigue, or other neurological symptoms — should be evaluated by a physician. Conditions including thyroid disorders, anemia, sleep apnea, autoimmune conditions, and early neurodegenerative disease can all present with cognitive symptoms. Never attribute worsening cognitive function solely to lifestyle without ruling out medical causes.
What is the fastest natural way to clear brain fog?
For acute brain fog — the kind that sets in during a long afternoon — the fastest interventions are physical movement (a 10–15 minute walk), cold water on the face and wrists, deliberate slow breathing for 3–5 minutes, and hydration. These directly address the immediate physiological contributors: reduced cerebral blood flow, dehydration, and sympathetic nervous system dominance. For chronic brain fog, there are no shortcuts — the underlying contributors need to be addressed systematically.
Is brain fog related to gut health?
Yes, significantly so. The gut-brain axis — the bidirectional communication network between the gastrointestinal tract and the central nervous system — plays a major role in cognitive function. The gut microbiome produces neuroactive compounds, modulates immune signaling, and communicates directly with the brain via the vagus nerve. Gut dysbiosis (microbiome imbalance), leaky gut (intestinal hyperpermeability), and inflammatory bowel conditions are all associated with increased incidence and severity of cognitive symptoms including brain fog.
What foods are worst for brain fog?
The dietary patterns most consistently associated with cognitive impairment are those high in refined sugars, ultra-processed foods, industrial seed oils, and alcohol. These inputs drive neuroinflammation through multiple mechanisms: glucose dysregulation impairs brain energy metabolism, industrial oils promote pro-inflammatory eicosanoid production, processed food additives disrupt the gut microbiome, and alcohol interferes with sleep architecture and B-vitamin status simultaneously.
Can stress alone cause brain fog?
Yes. Chronic psychological stress elevates cortisol levels, and sustained cortisol elevation directly impairs prefrontal cortex function — the brain region responsible for working memory, attention, and executive function. Stress also disrupts sleep architecture, increases gut permeability, and reduces the production of BDNF. In this way, stress does not just cause brain fog directly — it creates the physiological conditions that allow multiple other drivers of brain fog to take hold simultaneously.
Are nootropic supplements necessary to reduce brain fog?
No — not as a starting point. For most adults, the foundational lifestyle interventions (sleep quality, anti-inflammatory diet, regular aerobic exercise, stress management, hydration) will produce significant cognitive improvement without supplementation. Nootropics are most effective as an adjunct layer once lifestyle foundations are established, not as a substitute for them. That said, targeted supplementation for documented deficiencies (vitamin D, magnesium, B12, omega-3) can be a meaningful first step if blood work confirms deficiency.
Daniel Mercer is a health science writer specializing in cognitive performance, nootropics, and brain health research. With a background in biomedical sciences and over a decade reviewing clinical literature on mental performance and supplementation, he founded Cognitive Insight Lab to cut through the noise and deliver evidence-based analysis for people who take their cognitive health seriously. Daniel does not accept sponsored content and has no financial ties to the brands reviewed on this site.