Omega-3 for Brain Health: What the Science Really Says
⚠️ Important Notice: This article is for informational and educational purposes only. The information provided does not replace guidance from a qualified healthcare professional. For personal decisions related to your cognitive health, consult a licensed professional.
Omega-3 for brain health is one of the most researched topics in nutritional neuroscience — and one of the most misunderstood by the general public. The supplement industry has spent decades attaching sweeping cognitive promises to fish oil capsules. Meanwhile, the actual science tells a more nuanced, and in some ways more compelling, story.
The brain is nearly 60% fat by dry weight. A significant portion of that fat is DHA — docosahexaenoic acid, the long-chain omega-3 fatty acid that forms the structural backbone of neuronal membranes. Without adequate DHA, those membranes become less fluid, less efficient at transmitting signals, and more vulnerable to oxidative damage. This is not a wellness-blog assertion — it is established neurobiological fact, documented in research from institutions including Harvard Medical School, the National Institutes of Health, and the Framingham Heart Study.
Yet most American adults are chronically deficient in omega-3 fatty acids. According to data from the National Health and Nutrition Examination Survey (NHANES), fewer than 10% of US adults meet the recommended intake of omega-3s through diet alone. For adults between 35 and 60 — the age range when the earliest functional signs of cognitive aging typically emerge — that gap carries real consequences.
Disclaimer: This content is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare professional before following any recommendations, including changes to supplementation or diet.
This article examines what omega-3 fatty acids actually are, how they function in the brain at a mechanistic level, what the research genuinely supports (and what it doesn’t), how to assess your intake, and how to choose a supplement if you decide that’s the right step. The goal is to give you a complete, honest picture — not a sales pitch.
What Are Omega-3 Fatty Acids and Why Does the Brain Need Them?
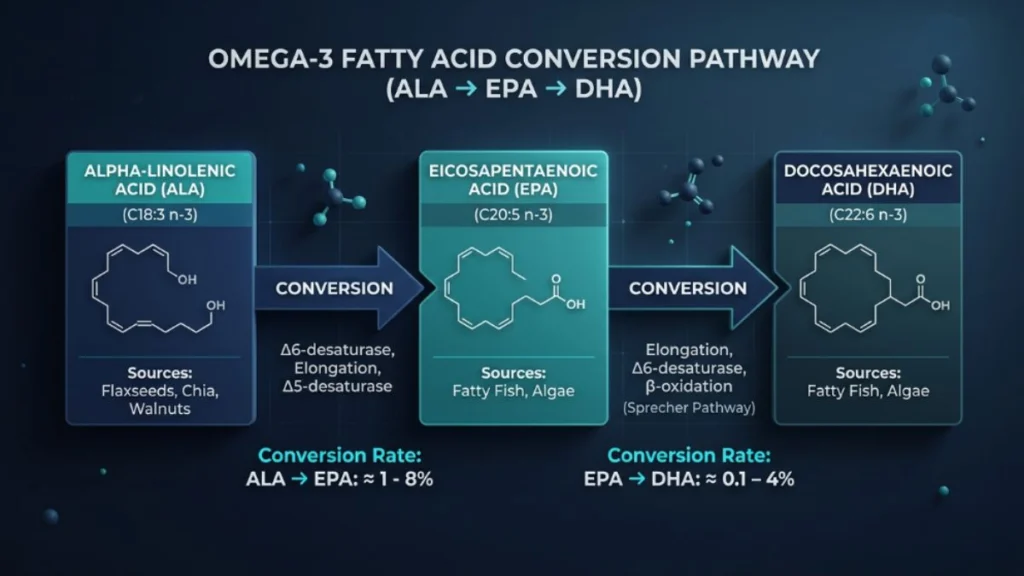
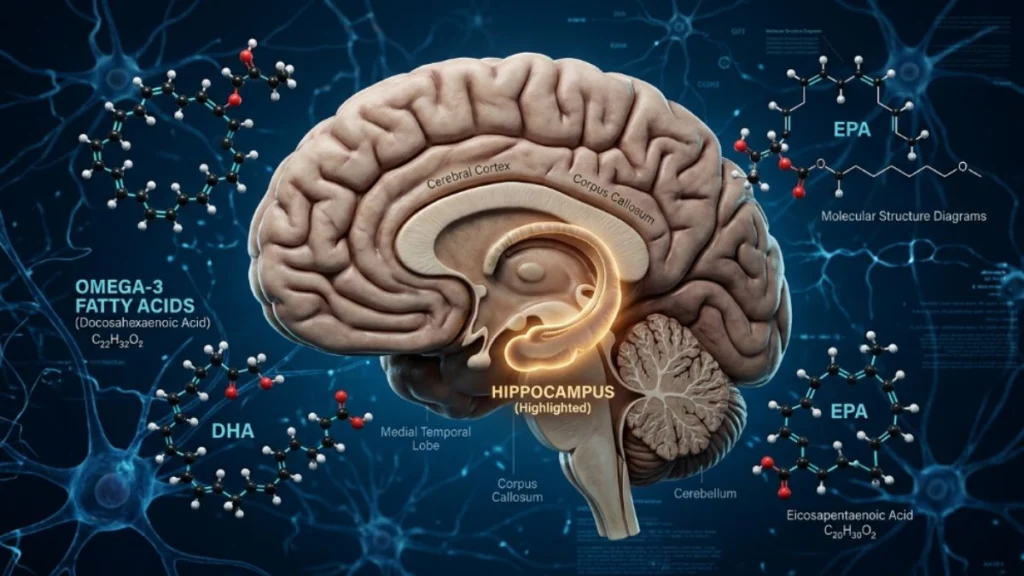
Omega-3 fatty acids are a family of polyunsaturated fats characterized by a double bond at the third carbon from the omega end of the fatty acid chain. The three primary omega-3s relevant to human health are:
- ALA (alpha-linolenic acid): Found in plant sources like flaxseed, chia seeds, and walnuts. It is an essential fatty acid — the body cannot produce it, so it must come from food or supplements.
- EPA (eicosapentaenoic acid): Found primarily in fatty fish and marine sources. It plays a central role in reducing neuroinflammation and supporting mood regulation.
- DHA (docosahexaenoic acid): The dominant structural omega-3 in the brain. It comprises approximately 97% of the omega-3 fatty acids found in the brain and 93% of those in the retina.
The Brain Is Structurally Dependent on DHA
Every neuron in the brain is encased in a cell membrane — a phospholipid bilayer that governs how efficiently the cell receives and transmits signals. DHA is the primary polyunsaturated fatty acid embedded in those membranes. Higher DHA content correlates directly with greater membrane fluidity, faster signal transmission, and more efficient synaptic function.
When DHA levels are insufficient, the brain substitutes other fatty acids into the membrane architecture — typically omega-6s, which are far more abundant in the standard American diet. This substitution produces stiffer, less fluid membranes, impaired neurotransmitter receptor function, and increased susceptibility to inflammation-driven neural damage.
The ALA Conversion Problem
A persistent misconception is that plant-based omega-3s adequately cover the brain’s DHA needs. The conversion rate from ALA to EPA is approximately 5–10%, and from ALA to DHA, it is less than 1% in most adults. For practical purposes, plant-sourced omega-3s do not meaningfully supply the brain with DHA. This matters most for vegetarians, vegans, and anyone relying on flaxseed oil supplements as their primary omega-3 source.
How Omega-3s Support Brain Function: The Four Key Mechanisms
Understanding how omega-3s actually work in the brain — not just that they “support brain health” — transforms how you evaluate both dietary choices and supplement claims.
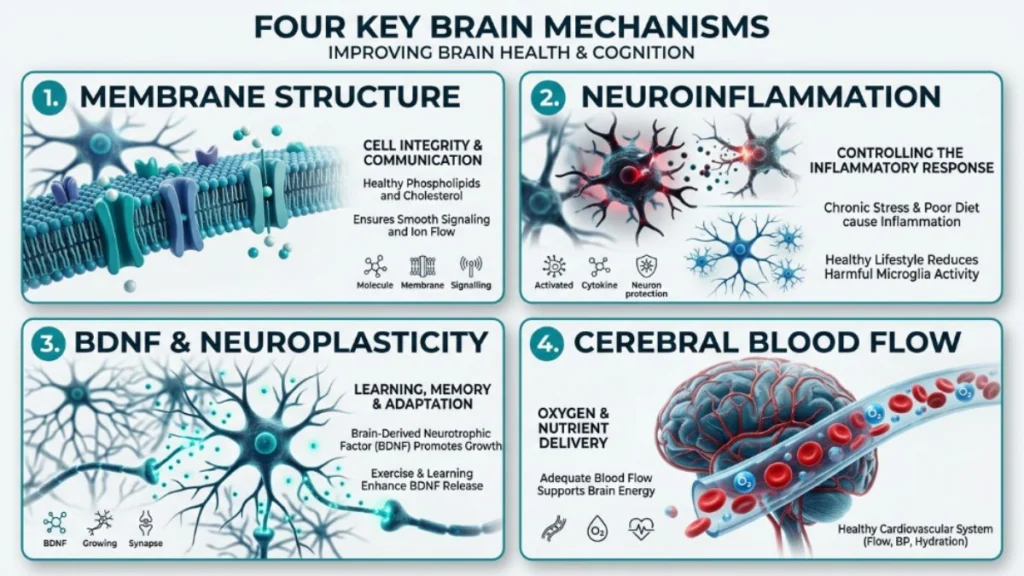
1. Structural Integrity of Neuronal Membranes
As described above, DHA is the structural foundation of neuronal cell membranes. Adequate DHA ensures those membranes remain fluid enough for efficient ion channel function, neurotransmitter receptor responsiveness, and synaptic vesicle release. This is a continuous maintenance function — not a one-time benefit — which is why consistent intake over time matters more than occasional supplementation.
2. Neuroinflammation Regulation
EPA is the primary omega-3 involved in modulating neuroinflammation. It serves as a precursor to specialized pro-resolving mediators (SPMs) — molecules that actively resolve inflammatory responses in neural tissue. Chronic low-grade neuroinflammation is increasingly recognized as a central mechanism in age-related cognitive decline, depression, and neurodegenerative disease pathology.
A landmark 2021 review published in Frontiers in Aging Neuroscience identified neuroinflammation as one of the primary modifiable contributors to cognitive aging, with omega-3 intake being among the best-studied dietary interventions for reducing it.
3. Neuroplasticity and BDNF Support
Brain-derived neurotrophic factor (BDNF) is often described as “fertilizer for the brain” — it supports the survival of existing neurons and promotes the growth of new neural connections. DHA has been shown to upregulate BDNF expression, particularly in the hippocampus, the brain region most directly involved in learning and memory.
Research from the University of California, Los Angeles, published in the Journal of Nutritional Biochemistry, demonstrated that DHA deficiency significantly reduces BDNF levels in the hippocampus, while DHA supplementation reverses this effect in both animal and preliminary human studies.
4. Cerebrovascular Health
EPA and DHA both support healthy blood flow by reducing platelet aggregation, improving endothelial function, and modestly reducing blood pressure and triglyceride levels. Cerebral blood flow — the delivery of oxygen and glucose to neurons — is a direct determinant of cognitive performance. What is consistently good for cardiovascular health is consistently good for cognitive health.
What the Research Actually Shows: Separating Signal from Noise
This is where honest analysis becomes essential. The omega-3 research landscape includes genuine findings and genuine disappointments — and both are worth understanding.
Where the Evidence Is Strong
Depression and mood regulation: The evidence for EPA’s role in mood disorders is among the most consistent in omega-3 research. A 2019 meta-analysis published in Translational Psychiatry, analyzing data from 26 clinical trials, found that omega-3 supplementation — particularly formulas with higher EPA content — produced significant reductions in depressive symptoms. Effects were most pronounced in people with confirmed inflammatory markers.
Age-related cognitive decline: The Framingham Heart Study tracked over 2,000 participants over 8 years and found that higher plasma DHA levels were associated with a 47% lower risk of developing all-cause dementia. The study, published in Archives of Neurology, remains one of the most cited pieces of evidence for the long-term neuroprotective value of adequate DHA.
Brain volume and atrophy: A 2012 study from Oregon Health & Science University found that participants with higher omega-3 blood levels had significantly larger brain volumes on MRI scans, including the hippocampus — with differences roughly equivalent to preserving 1–2 years of brain aging.
Where the Evidence Is More Mixed
Acute cognitive performance in healthy adults: Supplementation studies in cognitively healthy younger adults show modest and inconsistent results. Omega-3s appear most beneficial when baseline deficiency exists or when cognitive aging has already begun. Adding omega-3s to an already-optimized system produces smaller measurable gains.
Alzheimer’s disease treatment: Despite early promise from observational studies, randomized controlled trials using omega-3 supplementation in patients with established Alzheimer’s disease have shown limited benefit. The current scientific consensus suggests that omega-3s may be more valuable as a preventive intervention in earlier decades than as a treatment once significant neurodegeneration has occurred.
💡 Practical Tip: The most consistent cognitive benefits from omega-3 supplementation appear in populations with documented deficiency, elevated inflammatory markers, or existing mood difficulties — not necessarily in cognitively healthy adults at peak function. If you’re unsure of your status, an omega-3 index blood test (available through your physician or direct-to-consumer labs) provides a concrete baseline.
| Research Area | Evidence Quality | Key Finding |
|---|---|---|
| Depression / mood regulation | Strong (multiple RCTs and meta-analyses) | EPA-dominant formulas reduce depressive symptoms |
| Age-related cognitive decline | Strong (large longitudinal studies) | Higher DHA associated with 47% lower dementia risk (Framingham) |
| Brain volume / atrophy | Moderate-Strong | Higher omega-3 index linked to larger brain volume |
| Acute focus in healthy adults | Weak-Moderate | Inconsistent results; effects most pronounced in deficient populations |
| Alzheimer’s treatment | Weak | Limited benefit in established disease; stronger case for prevention |
| ADHD and attention | Moderate | Modest improvements in attention, particularly in children |
How Much Omega-3 Does the Brain Actually Need?
Recommended intakes vary by organization, individual health status, and the specific omega-3 being discussed. Here is a practical framework.
General Dietary Reference
The American Heart Association recommends at least two servings of fatty fish per week for cardiovascular health — roughly equivalent to 250–500 mg of combined EPA and DHA daily from food. For cognitive health specifically, several research institutions suggest a higher threshold is relevant.
The Global Organization for EPA and DHA Omega-3s (GOED) and several European nutrition bodies suggest 500 mg combined EPA+DHA daily for general health maintenance, with 1,000–2,000 mg daily being a common target in cognitive health research protocols.
The Omega-3 Index: A More Useful Metric
Rather than focusing on intake milligrams, the omega-3 index — a measure of EPA+DHA as a percentage of total red blood cell fatty acids — provides a more clinically meaningful picture. An omega-3 index of 8% or above is associated with the lowest cardiovascular and cognitive risk in the literature. Most Americans test at 4–5%.
Special Considerations
- Older adults (55+): Absorption efficiency decreases with age. Higher supplemental doses (2,000–3,000 mg EPA+DHA daily) are sometimes used in research protocols.
- Vegetarians and vegans: Plant-based ALA sources do not adequately substitute. Algae-derived DHA supplements are the appropriate alternative — they are the original marine source from which fish accumulate DHA.
- People with inflammatory conditions: Higher EPA is often prioritized; doses up to 4,000 mg EPA+DHA daily are used in clinical settings under physician supervision.
⚠️ Attention: At doses above 3,000 mg of EPA+DHA daily, omega-3s can affect platelet aggregation and may interact with anticoagulant medications including warfarin and aspirin. Anyone on blood thinners should consult their physician before beginning high-dose supplementation.
Dietary Sources vs. Supplementation: What Matters Most
The food-first argument is not just a wellness platitude — it has real nutritional logic behind it. Fatty fish provides EPA and DHA alongside a broader matrix of nutrients: selenium, vitamin D, protein, and phospholipid-bound omega-3s that may be absorbed more efficiently than the triglyceride form found in most supplements.
The Highest DHA and EPA Dietary Sources
- Wild salmon (Atlantic or sockeye): 1,500–2,200 mg EPA+DHA per 3 oz serving — among the most concentrated dietary sources available
- Mackerel: 2,200–2,400 mg EPA+DHA per 3 oz — the highest per-serving food source
- Sardines (canned in oil): 1,400–1,800 mg EPA+DHA per 3 oz — accessible, affordable, and consistently high
- Herring: 1,600–1,800 mg per serving — widely consumed in Northern Europe, underutilized in the US
- Anchovies: 400–500 mg per oz — practical in small quantities as a flavor addition
- Oysters: 500–700 mg per 3 oz — plus zinc and vitamin B12
Two to three servings of fatty fish per week — primarily wild-caught where accessible — covers most cognitively relevant omega-3 needs without supplementation for most healthy adults.
When Supplementation Makes Sense
Supplementation becomes relevant when:
- Fish consumption is consistently below two servings per week
- Diet is primarily plant-based
- Omega-3 index testing reveals deficiency (below 6%)
- Elevated inflammatory markers are present
- Cognitive aging symptoms are notable and lifestyle optimization has already been addressed
👉 If you’re also experiencing brain fog alongside low omega-3 intake, the picture is often broader than a single nutrient — this article covers the full landscape of contributing factors and what to address first:
Brain Fog Causes in Adults: What’s Really Behind the Mental Haze

🛒 Top Omega-3 Supplements for Brain Health on Amazon
Based on the criteria above — EPA/DHA ratios, triglyceride form, purity, and third-party testing — these are among the most consistently rated omega-3 supplements currently available on Amazon.
4.8★ · 6,900+ reviews · Molecularly distilled · 10,000+ bought last month · $7.60
View on Amazon →
4.7★ · 16,800+ reviews · EPA + DHA · 10,000+ bought last month · $12.49
View on Amazon →
4.7★ · 16,000+ reviews · Larger supply · Best value per serving · $14.69
View on Amazon →
⚠️ Disclosure: This page contains affiliate links. If you purchase through these links, we may earn a small commission at no extra cost to you. This does not influence our recommendations.
How to Choose an Omega-3 Supplement: What Actually Matters
The supplement market for omega-3s is enormous and inconsistent in quality. These are the criteria that distinguish an effective product from expensive marketing.
EPA vs. DHA Ratio: Match to Your Goal
- For cognitive structure and long-term brain health: DHA-dominant formula (higher DHA than EPA)
- For mood, depression, or neuroinflammation: EPA-dominant formula (EPA ≥ 2:1 ratio to DHA)
- For general brain and cardiovascular health: Balanced formula (roughly equal EPA and DHA)
Form Matters: Triglyceride vs. Ethyl Ester
Most budget fish oil supplements use the ethyl ester (EE) form — a processed form that studies show is absorbed 50–70% less efficiently than the natural triglyceride (TG) form. Re-esterified triglyceride (rTG) products cost more but deliver meaningfully better bioavailability.
Krill oil provides omega-3s in phospholipid form, which some research suggests may cross the blood-brain barrier more efficiently — though at lower absolute doses per gram than fish oil.
Purity and Oxidation: The Hidden Problem
Omega-3 supplements are highly susceptible to oxidation — the very process that makes them rancid. A 2015 Consumer Reports investigation and multiple independent analyses found that a significant proportion of commercially available fish oil products exceeded safe oxidation thresholds. Oxidized fish oil is not only less effective — it may be actively harmful, generating inflammatory byproducts.
Practical indicators of quality:
- Third-party testing certificates (IFOS, USP, NSF International)
- Packaging that limits light and oxygen exposure (dark glass or nitrogen-flushed packaging)
- A mild, clean smell — strong fishy odor indicates oxidation
- Clear expiration dates with reasonable shelf life from purchase
✅ Best Practice: When evaluating an omega-3 supplement, look specifically for third-party certification from the International Fish Oil Standards (IFOS) program. IFOS tests for EPA/DHA content accuracy, heavy metal contamination, PCBs, dioxins, and oxidation levels — and publishes the results publicly. A supplement without independent third-party certification provides far less certainty about what you’re actually getting.

Omega-3 Deficiency: Signs the Brain May Be Running Low
Because DHA deficiency develops gradually and has no single dramatic symptom, it is easy to overlook. These are the patterns that may indicate chronically inadequate omega-3 status — recognizing that each can have multiple causes and that professional evaluation is the appropriate response to persistent symptoms.
- Persistent difficulty concentrating or sustaining mental focus
- Increased frequency of low mood or emotional flatness
- Notable decline in memory recall, particularly for recent events
- Dry skin, brittle nails, or dry eyes (omega-3s support epithelial tissue broadly)
- Difficulty sleeping or disrupted sleep architecture
- Joint stiffness or increased systemic inflammation markers
None of these symptoms confirms omega-3 deficiency on its own. But when several occur together — particularly in the context of a diet low in fatty fish and high in omega-6s (vegetable oils, processed foods) — assessing omega-3 status through an index test provides a clear and actionable baseline.
👉 If these symptoms sound familiar alongside declining mental sharpness, it’s worth understanding the broader cognitive picture — this overview helps you assess where omega-3 fits within the full range of factors at play: Early Signs of Cognitive Decline: What Adults Should Know
Omega-3 and the Omega-6 Balance: The Context Most Articles Skip
No discussion of omega-3 for brain health is complete without addressing the ratio problem. The modern American diet provides omega-6 and omega-3 fatty acids in a ratio estimated at 15:1 to 20:1. Our evolutionary diet is estimated to have maintained a ratio closer to 4:1 or even 1:1.
This matters because omega-6 and omega-3 fatty acids compete for the same enzymatic pathways. When omega-6s dominate — as they do in a diet heavy in processed vegetable oils (corn, soybean, sunflower) — they suppress the synthesis and utilization of EPA and DHA even when intake is nominally adequate.
The practical implication: increasing omega-3 intake while simultaneously reducing omega-6 consumption produces a more favorable shift in brain fatty acid composition than either intervention alone. Replacing processed seed oils with olive oil, reducing fried and processed foods, and increasing fatty fish collectively address both sides of this ratio.
💡 Practical Tip: The most impactful single dietary change for improving brain omega-3 status in most American adults is not adding a supplement — it is replacing refined seed oils (corn, soybean, sunflower) in home cooking with extra-virgin olive oil, while adding 2–3 weekly servings of fatty fish. This addresses both omega-3 intake and the omega-6 displacement that prevents its use.
👉To see how omega-3 and other nutritional factors fit within a complete brain optimization strategy, this overview of evidence-based approaches covers the full picture:
How to Reduce Brain Fog Naturally: The Evidence-Based Approach

Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended to serve as medical advice, diagnosis, or treatment. Results may vary from person to person. If you have any medical conditions, are taking medications, or have health concerns, consult a licensed healthcare professional before making changes to your supplementation or dietary practices.
Frequently Asked Questions
How much omega-3 should I take daily for brain health?
For general cognitive maintenance, research protocols commonly use 1,000–2,000 mg of combined EPA+DHA daily. For mood support or neuroinflammation, higher EPA concentrations are often used in clinical studies, with total doses of 2,000–3,000 mg EPA+DHA. The most clinically meaningful target is an omega-3 index of 8% or above, measured via blood test. Starting with 1,000 mg combined EPA+DHA and testing your index after 3–4 months provides a personalized baseline rather than guessing at a fixed dose.
Is fish oil or krill oil better for the brain?
Both deliver EPA and DHA, but the form differs. Fish oil typically provides higher absolute doses per capsule at lower cost. Krill oil delivers omega-3s in phospholipid form, which some research suggests may cross the blood-brain barrier more efficiently and may be better tolerated by those who experience fish oil aftertaste. For most people, a high-quality, third-party-tested fish oil in triglyceride form provides excellent bioavailability at a more accessible price point. The difference between a high-quality fish oil and krill oil is less significant than the difference between a high-quality and a low-quality fish oil.
How long does it take to notice results from omega-3 supplementation?
Red blood cell omega-3 composition — the most meaningful marker of tissue levels — takes approximately 8–12 weeks to reach a new steady state after beginning supplementation. Most people do not notice acute changes in the first 2–4 weeks. Mood-related effects from EPA tend to appear earlier than structural or memory-related effects. Plan for a 3-month consistent trial before evaluating results, and consider an omega-3 index test at baseline and after 3 months for an objective measure.
Can vegetarians and vegans get enough omega-3 for brain health?
The short answer is not easily through diet alone. ALA from plant sources (flaxseed, chia, walnuts) converts to DHA at less than 1% efficiency in most adults. Algae-derived DHA is the effective solution — algae is the primary marine DHA source, and fish accumulate their DHA by eating algae. Algae-based omega-3 supplements provide direct DHA (and some EPA) without the fish. This is the preferred recommendation for plant-based eaters who want to maintain adequate brain DHA status.
What are the side effects of omega-3 supplements?
At commonly recommended doses (1,000–3,000 mg EPA+DHA daily), omega-3 supplements are generally well tolerated. The most frequent side effect is fishy aftertaste or mild gastrointestinal discomfort, which is largely addressed by choosing high-quality, low-oxidation products and taking them with meals. At higher doses (above 3,000 mg daily), omega-3s may reduce platelet aggregation and should be used cautiously by anyone taking anticoagulants. High-dose supplementation should always be discussed with a healthcare provider.
Does cooking fish destroy its omega-3 content?
Cooking reduces omega-3 content modestly, but does not eliminate it. Baking, poaching, and steaming preserve the most EPA and DHA — losses are typically in the 10–20% range. Frying at high heat causes the greatest degradation and adds back oxidized cooking oils that counteract omega-3 benefits. Canned salmon and sardines retain approximately 70–80% of their original omega-3 content and represent one of the most practical and accessible dietary omega-3 sources available. Eating canned sardines twice weekly is nutritionally more impactful than most over-the-counter supplements.
Are omega-3s safe for older adults with heart conditions?
In general, yes — EPA and DHA are cardioprotective at standard supplemental doses and are recommended by the American Heart Association for adults with documented heart disease. However, the specific interaction with anticoagulant medications (warfarin, clopidogrel, novel anticoagulants) requires physician oversight, particularly at doses above 1,000 mg daily. Any older adult managing cardiovascular disease should discuss omega-3 supplementation with their cardiologist or primary care physician before starting or increasing doses.
Daniel Mercer is a health science writer specializing in cognitive performance, nootropics, and brain health research. With a background in biomedical sciences and over a decade reviewing clinical literature on mental performance and supplementation, he founded Cognitive Insight Lab to cut through the noise and deliver evidence-based analysis for people who take their cognitive health seriously. Daniel does not accept sponsored content and has no financial ties to the brands reviewed on this site.