Early Signs of Cognitive Decline: What Adults Should Know
⚠️ Important Notice: This article is for informational and educational purposes only. The information provided does not replace guidance from a qualified healthcare professional. For personal decisions related to your cognitive health, please consult a licensed medical professional.
The early signs of cognitive decline are often subtle enough to dismiss — until they aren’t. You misplace your keys for the third time this week. You lose your train of thought mid-sentence in a meeting. You walk into a room and stand there for a long moment, completely blank. It feels like a bad day. Then it happens again.
For millions of American adults between 35 and 60, these moments are becoming harder to ignore. According to the Centers for Disease Control and Prevention (CDC), approximately 1 in 9 Americans over 45 reports experiencing some form of subjective cognitive decline — defined as self-reported worsening of memory or thinking. That number is almost certainly an undercount, because most people wait years before mentioning it to a doctor.
The frustrating part is that early cognitive changes don’t arrive with a clear label. They blend into the noise of modern life: the stress, the poor sleep, the relentless multitasking. It becomes genuinely difficult to tell where “normal aging” ends and something worth paying attention to begins.
Disclaimer: This content is for informational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider before making changes to your diet, supplements, or cognitive health routine.
That distinction — between benign forgetfulness and early cognitive decline — is exactly what this article addresses. You’ll learn what the research says about the earliest warning signals, which symptoms deserve closer attention, what risk factors are within your control, and when it’s time to speak with a healthcare professional. The goal is to give you clarity, not alarm.
What Does “Cognitive Decline” Actually Mean?
Cognitive decline refers to a measurable reduction in one or more areas of mental function — including memory, attention, language, reasoning, and processing speed. It exists on a spectrum, and understanding that spectrum matters enormously.
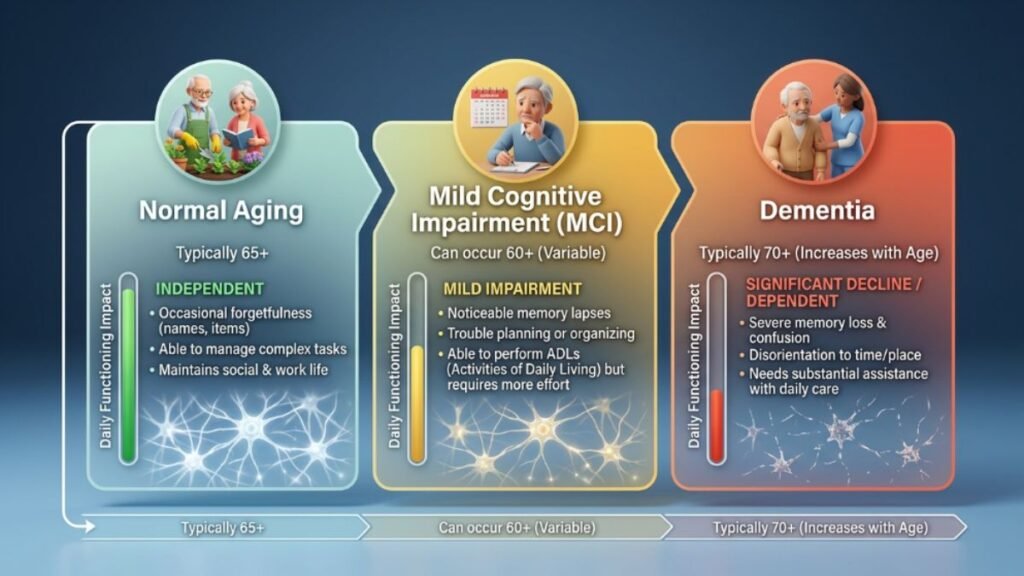
The Spectrum: Normal Aging vs. MCI vs. Dementia
Not all cognitive changes are equal. Researchers and clinicians typically distinguish between three categories:
Age-related cognitive changes are considered normal. Reaction time slows modestly with age. Retrieving a specific name or word may take a few seconds longer than it did at 30. These changes do not interfere significantly with daily life.
Mild Cognitive Impairment (MCI) sits in the middle ground. It involves measurable decline beyond what’s expected for age and education level, but not severe enough to disrupt independent functioning. MCI affects an estimated 15–20% of adults over 65, according to the Alzheimer’s Association — but it can begin showing signs years or even decades earlier.
Dementia (including Alzheimer’s disease) represents a more advanced stage where cognitive changes are severe enough to impair daily activities, relationships, and self-care.
The critical point is this: most cognitive decline doesn’t begin in old age. Research published in Neurology has shown that certain biomarkers of Alzheimer’s disease can be detectable in the brain 20 or more years before symptoms become obvious. The early warning window is real — and it matters.
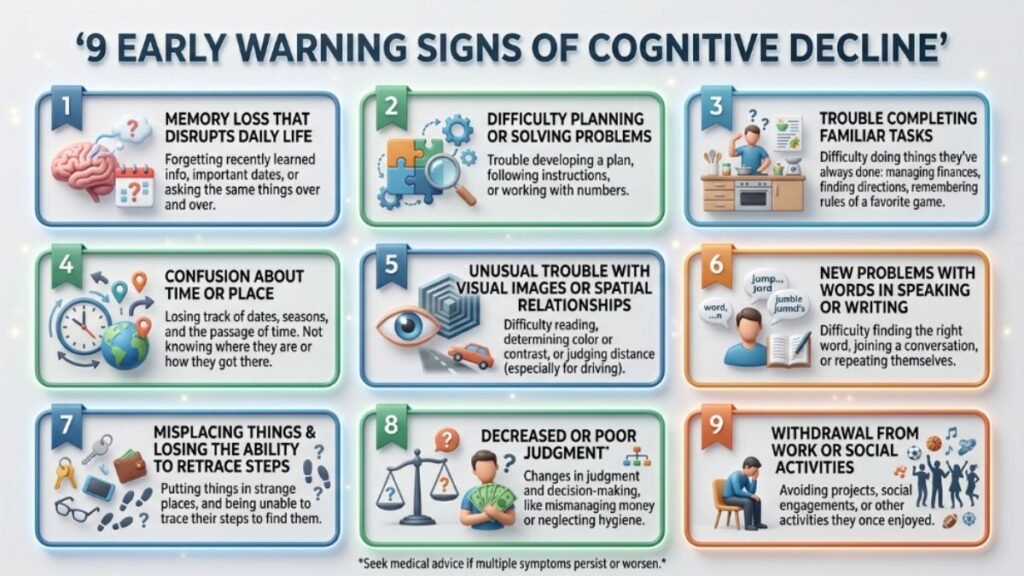
The 9 Early Signs of Cognitive Decline Adults Often Overlook
These are the signals that research consistently identifies as early — not the dramatic memory loss of late-stage dementia, but the quieter changes that tend to precede it by years.
1. Forgetting Recent Events More Than Older Ones
One of the most characteristic early patterns is difficulty retaining new information while older memories remain sharp. You remember your childhood phone number perfectly but can’t recall what you had for breakfast or what was discussed in yesterday’s meeting.
This asymmetry — sparing remote memories while struggling with recent ones — reflects early changes in the hippocampus, the brain region most directly involved in forming new memories. It’s a different experience from ordinary forgetfulness, which tends to affect all time periods equally.
2. Losing the Thread Mid-Conversation
Difficulty following or maintaining complex conversations is an underreported early sign. This isn’t about losing your train of thought occasionally — everyone does that. The pattern to watch is when it becomes consistent: you start a sentence and genuinely can’t retrieve how you intended to finish it, or you follow the first half of a conversation but lose context as it continues.
This relates to working memory — the brain’s capacity to hold and manipulate information in real time. Working memory shows measurable decline in the earliest stages of cognitive change, often before episodic memory is noticeably affected.
3. Difficulty with Familiar Tasks
Struggling with tasks that were once automatic is a meaningful signal. Getting confused while following a recipe you’ve made dozens of times. Needing to look up directions to a place you’ve driven to for years. Making errors in routine spreadsheet work that you would never have made before.
The brain’s procedural and executive systems are being asked to compensate for reduced automatic processing — and the effort shows.
4. Mood and Personality Shifts Without Clear Cause
Emerging research increasingly links early cognitive decline with changes in mood and temperament that often precede obvious memory symptoms. Increased irritability, social withdrawal, anxiety, or apathy — particularly when these represent a change from baseline — can reflect early neurochemical shifts, especially in the prefrontal cortex.
A 2022 study published in Frontiers in Aging Neuroscience found that neuropsychiatric symptoms, including depression and anxiety, were among the earliest predictors of progression from normal cognition to MCI.
💡 Practical Tip: If someone close to you has noticed personality changes you haven’t recognized in yourself, take that seriously. Early cognitive changes are often more visible to others than to the person experiencing them.
5. Getting Easily Overwhelmed by Complexity
Tasks that require managing multiple variables at once — planning a trip, organizing a project, managing finances — become disproportionately exhausting. The mental load that used to feel manageable now produces frustration, avoidance, or errors.
This reflects reduced executive function, which encompasses planning, sequencing, mental flexibility, and impulse control. Executive function is controlled primarily by the prefrontal cortex, and it’s among the first cognitive domains to show age-related change.
6. Increased Difficulty Finding Words
The “tip-of-the-tongue” phenomenon — knowing you know a word but being unable to retrieve it — becomes notably more frequent. This goes beyond the occasional blank; it happens multiple times per day, with words that should be well within your vocabulary.
Word-finding difficulty (anomia) is one of the earliest and most reliable indicators of language-related cognitive change. When it increases in frequency and begins affecting professional or social communication, it warrants attention.
7. Losing Track of Time or Sequence
Confusion about what day it is, what month or season it is, or how much time has passed is a recognized early sign. This is different from being briefly disoriented after a poor night’s sleep — it involves a more persistent difficulty orienting to time.
Similarly, difficulty remembering the sequence of recent events (“Did that happen yesterday or last week?”) reflects disruption in temporal processing, which is hippocampus-dependent.
8. Reduced Concentration and Mental Stamina
The ability to sustain deep focus for extended periods — reading a complex book, working through a difficult problem, following a long argument — noticeably decreases. Mental fatigue arrives faster and is harder to recover from.
This isn’t burnout alone. While chronic stress and burnout cause similar symptoms, early cognitive decline produces a more persistent attentional fragility that doesn’t fully resolve with rest.
9. Repeating Yourself or Asking the Same Questions
Telling the same story to the same person within a short time frame, or asking the same question multiple times in a single conversation, is one of the more socially visible early signs. It reflects difficulty encoding the memory that a piece of information has already been communicated or received.
Normal Forgetting vs. Something More: A Practical Comparison
Understanding the difference between ordinary forgetfulness and early cognitive decline can save years of unnecessary anxiety — or help you act sooner when action matters.
| Situation | Likely Normal | Worth Monitoring |
|---|---|---|
| Forgetting a name temporarily | Recall comes back later | Name never comes back |
| Misplacing keys occasionally | You retrace your steps and find them | You find them in an unusual place and don’t remember putting them there |
| Forgetting a word momentarily | You find it within seconds | Happens multiple times daily, affects communication |
| Feeling mentally foggy after poor sleep | Clears after rest | Persists regardless of sleep quality |
| Missing an appointment once | Isolated incident | Happens repeatedly despite reminders |
| Having trouble with a new device | You learn with some effort | Familiar technology becomes confusing |
| Mood changes during stress | Resolves when stress resolves | Persistent change in personality baseline |
⚠️ Attention: This table is a general educational guide and not a diagnostic tool. Only a qualified healthcare professional can assess whether changes in your cognition are clinically significant.
Risk Factors That Accelerate Cognitive Decline
Not all risk factors are equal — and not all are outside your control. Understanding this distinction is one of the most actionable things you can do.
Modifiable Risk Factors
Research from the Lancet Commission on Dementia Prevention identifies a substantial proportion of dementia risk as modifiable — meaning lifestyle changes can meaningfully reduce it. Key modifiable factors include:
- Chronic sleep deprivation: Sleep is when the brain clears metabolic waste, including amyloid beta — a protein linked to Alzheimer’s pathology. Consistently sleeping fewer than 6 hours per night is associated with significantly elevated dementia risk.
- Physical inactivity: Aerobic exercise increases brain-derived neurotrophic factor (BDNF), a protein that supports neuron survival and growth. Regular exercise is one of the most evidence-backed interventions for preserving cognitive function.
- Cardiovascular risk factors: Hypertension, type 2 diabetes, and high LDL cholesterol are all independently associated with accelerated cognitive aging. What’s bad for the heart is reliably bad for the brain.
- Social isolation: Reduced social engagement is linked to faster cognitive decline, likely through reduced cognitive stimulation and increased chronic stress.
- Chronic stress: Elevated cortisol over long periods damages hippocampal tissue, directly impairing memory formation and recall.
- Poor nutrition: Diets high in ultra-processed foods and low in omega-3 fatty acids, antioxidants, and B vitamins are associated with poorer cognitive aging outcomes.
Non-Modifiable Risk Factors
- Age: Risk increases significantly after 65, though early-onset cases occur in people as young as their 40s.
- Family history and genetics: Having a first-degree relative with Alzheimer’s increases risk. The APOE-e4 gene variant is the most studied genetic risk factor, though carrying it does not guarantee disease development.
- Prior head injuries: A history of traumatic brain injury is associated with elevated long-term risk.

💡 Practical Tip: The Lancet Commission estimates that addressing 12 modifiable risk factors could prevent or delay up to 40% of global dementia cases. The earlier lifestyle changes begin, the greater their protective impact.
👉 If you’re ready to act on what you just read, this guide breaks down the most effective evidence-based strategies in practical, day-by-day terms:
How to Reduce Brain Fog Naturally
When to Talk to a Doctor
Most people experiencing the signs listed above wait too long before seeking a professional evaluation. The reluctance is understandable — there’s fear about what an evaluation might reveal, and a persistent hope that it’s just stress or fatigue.
Here’s the honest framework: if cognitive changes are affecting your daily life, your relationships, or your professional performance — and they are not clearly explained by an acute cause like illness or extreme sleep deprivation — a conversation with your doctor is appropriate.
A primary care physician can perform initial cognitive screening using validated tools such as the MoCA (Montreal Cognitive Assessment) or the Mini-Mental State Examination (MMSE). These aren’t definitive diagnoses — they’re starting points.
If screening suggests further evaluation, a referral to a neurologist or neuropsychologist is the next step. A comprehensive neuropsychological evaluation can map your cognitive profile across multiple domains and provide a meaningful baseline for monitoring change over time.
⚠️ Attention: Sudden or rapid cognitive changes are a medical emergency. If symptoms appear abruptly — especially alongside headache, vision changes, speech difficulty, or confusion — seek emergency care immediately. These may indicate stroke or another acute neurological event.
What an Early Evaluation Can Give You
- Clarity: Ruling out reversible causes (thyroid dysfunction, B12 deficiency, medication side effects, sleep apnea) that are frequently mistaken for early cognitive decline.
- A baseline: Establishing where you are neuropsychologically now makes future monitoring far more meaningful.
- Access to interventions: If MCI is identified, early interventions — lifestyle, medical, and cognitive — are more effective than those initiated after significant decline.
👉 Before you reach for any supplement, it pays to understand what the research actually supports — and what it doesn’t:
What Are Nootropics? A Science-Based Overview
Conditions That Mimic Cognitive Decline
Several reversible and treatable conditions produce symptoms that closely resemble early cognitive decline. Before assuming neurodegeneration, these should be ruled out:
| Condition | Cognitive Symptoms Produced | How It’s Identified |
|---|---|---|
| Hypothyroidism | Memory difficulties, mental fog, slowed thinking | TSH blood test |
| Vitamin B12 deficiency | Memory problems, confusion, mood changes | Blood panel |
| Sleep apnea | Daytime cognitive impairment, poor concentration | Sleep study |
| Depression | Pseudodementia — memory loss, confusion, slowed processing | Clinical evaluation |
| Medication side effects | Variable, depending on drug class | Medication review |
| Chronic stress / burnout | Attentional difficulties, working memory impairment | Clinical history |
Many people receive a cognitive decline evaluation and discover that their symptoms are explained entirely by one of these conditions — and that treatment produces meaningful improvement. This is a genuinely common and reversible scenario.

👉 Not sure whether what you’re experiencing is cognitive decline or something more reversible? This breakdown will help you tell the difference:
Brain Fog Causes in Adults: What’s Really Behind the Mental Haze
What You Can Do Right Now
Research into cognitive protection is robust enough to support clear, evidence-based actions. None of these are surprising — but the consistency of the evidence behind them is worth taking seriously.
The Most Protective Habits for Cognitive Longevity
Sleep (7–9 hours consistently): This is the single most impactful modifiable factor for brain health. Prioritize sleep quality as non-negotiable, not optional.
Aerobic exercise (150 minutes per week minimum): Even brisk walking produces measurable increases in hippocampal volume. Resistance training adds complementary benefits for executive function.
Cognitive engagement: Learning new skills, reading complex material, engaging in strategic games, and pursuing intellectually demanding work all support neuroplasticity — the brain’s capacity to form and strengthen connections.
Social connection: Regular meaningful social interaction is independently neuroprotective. Isolation is a risk factor; community is protective.
Nutritional quality: The Mediterranean diet and the MIND diet (Mediterranean-DASH Intervention for Neurodegenerative Delay) both have substantial research support for cognitive protection. Key elements include fatty fish, leafy greens, berries, olive oil, nuts, and reduced ultra-processed food intake.
Stress management: Chronic cortisol elevation is directly neurotoxic. Any consistent practice that reduces physiological stress — meditation, breathing practices, time in nature, regular exercise — contributes to cognitive protection.

👉 The science behind that capacity is more compelling — and more actionable — than most people expect: Neuroplasticity in Adults: How Your Brain Can Still Change
🛒 Foundational Supplements for Long-Term Brain Protection
Vitamin D3 deficiency is one of the most common and correctable risk factors for cognitive decline. These are among the most consistently rated D3+K2 supplements currently available on Amazon — a foundational starting point for anyone serious about long-term brain health.
4.8★ · 12,000+ reviews · 1,000 IU D3 + 45mcg K2 · 20,000+ bought last month · $8.96
View on Amazon →
4.7★ · 9,600+ reviews · High-potency formula · 40,000+ bought last month · $13.52
View on Amazon →
4.7★ · 4,600+ reviews · D3 + K1 + K2 + Iodine · 7,000+ bought last month · $18.00
View on Amazon →
⚠️ Disclosure: This page contains affiliate links. If you purchase through these links, we may earn a small commission at no extra cost to you. This does not influence our recommendations.
Conclusion
The early signs of cognitive decline are rarely dramatic. They tend to arrive quietly — a word that won’t come, a familiar route that suddenly requires effort, a conversation that slips away before it’s finished. Recognizing these patterns early is not about catastrophizing. It’s about giving yourself the most valuable thing available: time to act.
The research is clear on several fronts. Many apparent cognitive symptoms have reversible causes. Lifestyle factors that protect brain health are well-established and accessible. Early evaluation provides clarity, rules out treatable conditions, and establishes a baseline that makes future monitoring meaningful.
The brain is not a fixed organ. It responds to how you sleep, move, eat, engage, and manage stress — throughout your entire life. The most important cognitive health decisions are often the ones made years before symptoms become undeniable.
If anything in this article resonated with your experience, bring it to a conversation with your healthcare provider. Not with alarm — with information and intention.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended as medical advice, diagnosis, or treatment. Results and experiences vary between individuals. If you have a medical condition, are taking medication, or have concerns about your cognitive health, consult a licensed healthcare professional before making any changes.
Frequently Asked Questions
What is the most common early sign of cognitive decline?
Memory difficulty with recent events — particularly retaining newly learned information while older memories remain intact — is one of the most consistently reported early signs. Other early indicators include word-finding difficulty, reduced working memory, and increased difficulty with complex tasks that were previously automatic. These signs are worth monitoring when they occur frequently and represent a noticeable change from your personal baseline.
At what age does cognitive decline typically begin?
Subtle cognitive changes can begin as early as the late 30s or 40s, though they are rarely noticeable at that stage. Research published in Neurology and PNAS suggests that certain brain changes underlying late-life dementia begin decades before clinical symptoms appear. More perceptible changes typically emerge in the 50s and 60s for most people, but early action — adjusting lifestyle factors — is most effective when taken before symptoms become significant.
Is occasional forgetfulness a sign of early cognitive decline?
Not on its own. Occasional forgetting is a normal feature of how human memory works — the brain actively filters and deprioritizes information to function efficiently. The distinction is pattern, frequency, and functional impact. Forgetting where you put your phone once is unremarkable. Consistently forgetting conversations you had hours ago, or finding that memory lapses are beginning to affect your work or relationships, warrants attention.
Can cognitive decline be reversed or stopped?
True neurodegeneration — as in Alzheimer’s disease — cannot currently be reversed with available treatments, though significant research is ongoing. However, many causes of cognitive symptoms are reversible (see the conditions table above). And for age-related decline and early MCI, robust evidence supports lifestyle interventions — exercise, sleep, nutrition, cognitive engagement, stress management — in slowing progression and, in some cases, improving function. Early action produces far better outcomes than waiting.
What tests are used to detect early cognitive decline?
Initial screening typically involves brief validated tools like the MoCA (Montreal Cognitive Assessment) or MMSE (Mini-Mental State Examination), administered by a primary care physician. For more detailed evaluation, neuropsychological testing maps function across multiple cognitive domains and establishes a baseline. Imaging (MRI or PET scan) and blood biomarkers may be used in specialist settings. If you’re concerned, the first step is a conversation with your primary care provider.
How is cognitive decline different from normal aging?
Normal aging produces modest, gradual changes that do not meaningfully interfere with daily life — slightly slower word retrieval, mildly reduced multitasking capacity, occasional tip-of-the-tongue moments. Cognitive decline, by contrast, involves measurable reduction in function that affects real-world tasks, relationships, or professional performance. The distinction is one of degree, frequency, and functional impact rather than a sharp categorical line — which is why professional evaluation matters when you’re unsure.
Can stress and anxiety cause symptoms that look like cognitive decline?
Yes, significantly so. Chronic stress, anxiety, and depression are among the most common reversible causes of cognitive symptoms in adults under 65. Elevated cortisol directly impairs hippocampal function, and attentional systems are particularly sensitive to psychological stress. This is why addressing mental health is not separate from cognitive health — they are deeply interconnected. If cognitive symptoms appeared alongside or after a period of significant stress or mental health difficulty, that context is clinically important.
Daniel Mercer is a health science writer specializing in cognitive performance, nootropics, and brain health research. With a background in biomedical sciences and over a decade reviewing clinical literature on mental performance and supplementation, he founded Cognitive Insight Lab to cut through the noise and deliver evidence-based analysis for people who take their cognitive health seriously. Daniel does not accept sponsored content and has no financial ties to the brands reviewed on this site.